Typically, around a third of New Yorkers rely on Medicaid for health coverage, which is one of the highest levels of enrollment in the country. Over the past year, however, the economic downturn has caused enrollment to swell by about 10%, which has raised the cost of the program at a time when the state finds itself under fiscal pressure, with a projected deficit of $60 billion over the next four years.
At the onset of the pandemic, the Families First Coronavirus Response Act established a 6.2% increase in the federal Medicaid matching rate that helps fund the program, which has provided the state with a temporary lifeline. Concerns about the program’s fiscal sustainability, however, predate the coronavirus pandemic.
In recent years, program costs had been rising more than the state publicly acknowledged, but it wasn’t until the summer of 2019 that the discrepancy came to light: Actual costs had increased 12% rather than the 4% that the state had budgeted. Earlier in the year, the state had postponed a $1.7 billion payment from March to April in order to maintain the appearance that the program had stayed on budget during the previous fiscal year.
“The state had allowed costs to spiral beyond what the budget said they should be and, in addition to that, they hadn’t been transparent about it,” said Bill Hammond, a senior fellow for health policy at Empire Center for Public Policy, a fiscally conservative think tank. “They just let that problem fester and disguised what was going on.”
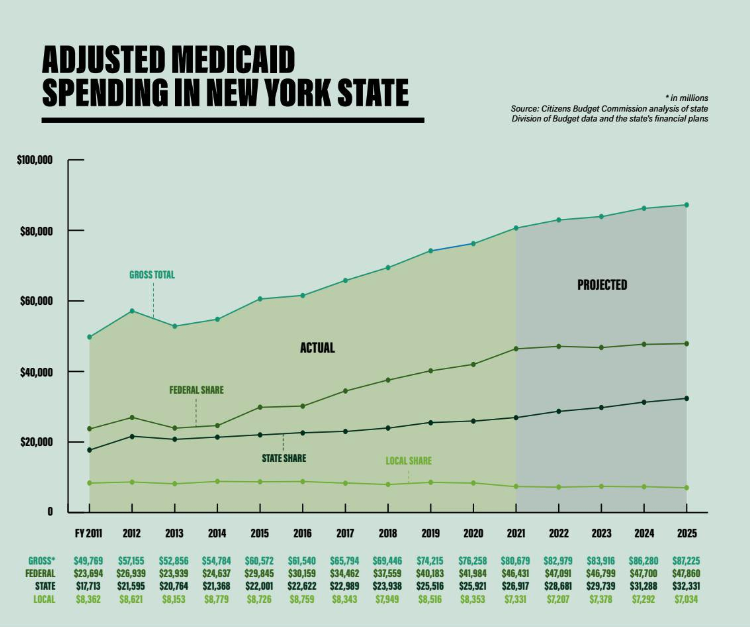
After the budgetary imbalance was revealed, the governor reconvened the Medicaid Redesign Team, which during his first term had recommended a global cap on outlays to limit the state-funded portion of the program’s costs. To realign true costs with the budgeted amount the second MRT would need to identify savings of around $2.5 billion per year, but at the time the pandemic struck the state was still falling short of that target by about $1 billion.
In addition to precipitating a jump in Medicaid enrollment, the pandemic also caused shifts in care. In the executive budget released in January, the state noted that it had gained savings from lower utilization, yet total Medicaid spending is still projected to grow 8.4% this fiscal year – with New York on the hook for 3.6% of that increase – which raises concerns about how the state will fund the program once the enhanced federal matching comes to an end.
“That is obviously fiscally unsustainable – our revenues don’t grow like that – but what is the cause?” said Andrew Rein, president of the Citizens Budget Commission, a nonpartisan fiscal monitor. “Because the information is not being provided in detail, we can’t separate it into its components to see what has to do with care cost increasing, and what has to do with the number of people we’re serving.”
Rein said that in areas such as long-term care and personal-care services, New York bore unusually high costs when compared with other states, but a lack of transparency around the program prevented outside observers from being able to make any assessments.
As budget watchdogs sound the alarm over rising costs, progressives claim that the real problem with Medicaid is that the state is spending too little on the program. Richard Gottfried, chair of the Assembly Health Committee, argues that the program has “suffered for years from underfunding.”
“In New York, Gov. Cuomo got us to enact a cap on Medicaid spending which has no relation to the true costs of health care,” he said.
Lara Kassel, the coordinator of Medicaid Matters, a statewide coalition that advocates for Medicaid recipients, told City & State that the program should have the flexibility to grow in order to “accommodate the needs of New Yorkers” and ensure that safety-net hospitals are adequately funded. Kassel, who served on the first Medicaid Redesign Team, dismissed the global cap as “arbitrary.”
“Health care costs have been rising for a whole host of reasons, but Medicaid should not be a target for keeping costs at bay,” Kassel said. “Medicaid is not the reason health care costs are high.”